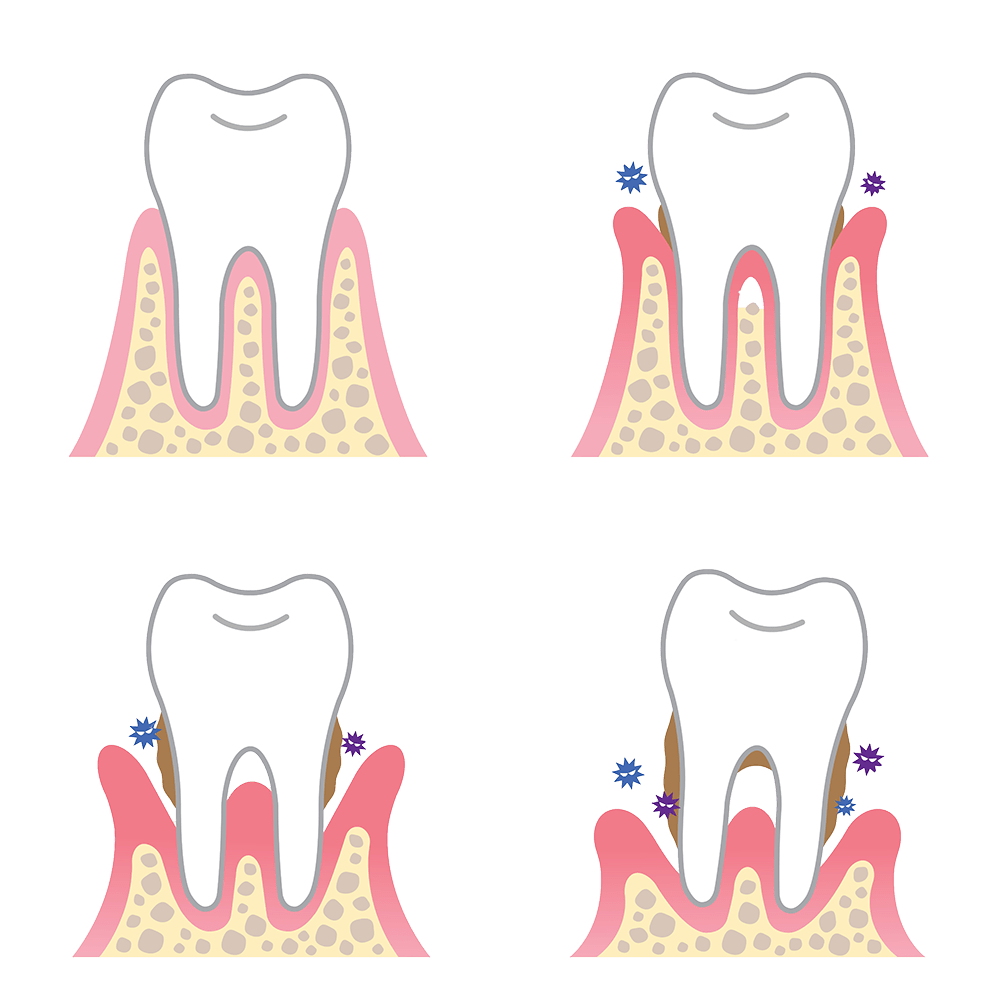
Periodontal disease (periodontitis) affects millions of adults in Australia, who have some form of this inflammatory condition of the gums. If left untreated, periodontal disease can result in irreversible damage to the connective ligaments and hard tissue that anchor, protect, nourish and support your teeth. The collective term used to describe these tissues is the periodontium or the periodontal structures – which is where periodontal disease gets its name.
First, there’s plaque and tartar
The process of gum disease and degeneration usually begins at the gum line. Your periodontal structures attach to your teeth a little below the gum line, and above them is a small space between your teeth and gums called a sulcus. When food gets trapped in a sulcus, plaque can form and eventually harden into tartar (calculus) which is much harder to brush and floss.
With your toothbrush rendered largely ineffective, bacterial plaque can penetrate the sulcus, and spread towards your tooth roots. Since the plaque is now developing below the gum line, you can no longer access and clean it off as usual with a toothbrush. This area provides ideal niches for oral bacteria to colonise and develop into a bacterial microflora or bacterial community – in other words, your gums are getting infected by bacteria.
Bacterial colonisation below the gum line
Over time, the microflora can evolve and grow to accommodate 1000s of new species of bacteria. For example, bacteria such as T. denticola and P. gingivalis are just two of a whole array of pathological disease-causing bacteria.
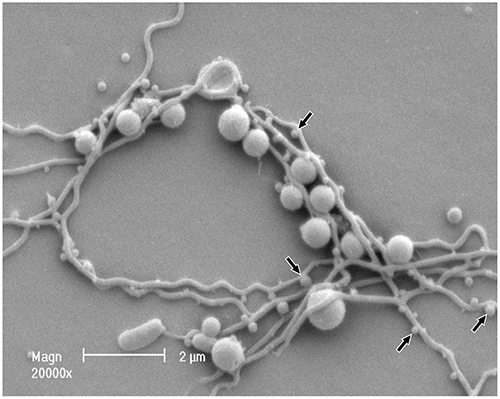
Above: Scanning electron micrograph of P. gingivalis and T. denticola*
These more complex, sophisticated bacteria can release enzymes and toxins that attack and break down the periodontium and your bone tissue. Many of them are motile – meaning they can “swim” with the use of flagella, or move using appendages along your tooth root surfaces.
Gingivitis, considered an earlier stage of periodontal disease and still easy to treat by your dentist, is an inflammation of your gums around the “necks” of your teeth. Inflammation is usually caused by a gums infected by pathogenic oral bacteria. Signs and symptoms include puffy, red, swollen, tender and inflamed gums that bleed easily, as well as gum abscesses.
Periodontal pockets and the loss of tooth support structures
If gingivitis is left untreated, pockets of space can develop between your teeth and gums in the infected areas. These pockets are called periodontal pockets, and are teeming with bacteria. Left untreated, periodontal pockets can continue to expand, while causing root cavities and bone loss, destroying connective tissue (periodontal structures), and separating tooth surfaces from the gum along the way.
As part of the body’s immune response, Mast cells are produced which attack good and bad cells, which results in further gum recession, and loss of gum tissue. This stage marks the progression from gingivitis to periodontal disease.
Tooth loss
At first, your teeth may become unstable and start to loosen and wobble. Then they can drift and move out of their sockets. Once the periodontal support structures give way altogether, your teeth start to detach from your gums.
At this point, affected teeth are no longer supported, and may fall out or require a dental extraction – if root canal therapy isn’t a viable dental option to save them.
Prevention
Fortunately, periodontal disease and tooth loss are almost entirely preventable.
Through regular brushing and flossing, you can keep your tooth surfaces clean and free of plaque for your entire life. Don’t forget your six-monthly dental check-up and clean, and if you are unsure of how to remove hard-to-reach plaque, ask your dentist for advice!
* Image credit: © 2014 Tan KH, Seers CA, Dashper SG, Mitchell HL, Pyke JS, Meuric V, et al. (2014) Porphyromonas gingivalis and Treponema denticola Exhibit Metabolic Symbioses. PLoS Pathog 10(3): e1003955. https://doi.org/10.1371/journal.ppat.1003955